On 28 May 2024, the Social Science in Humanitarian Action Platform (SSHAP) organised a roundtable discussion on the mpox (formerly known as monkeypox) outbreak which has been spreading in the Democratic Republic of the Congo (DRC) since early 2023.1 The objective was to appraise the current situation, with a particular focus on social science insights for informing context-sensitive risk communication and community engagement (RCCE) and wider operational responses.
The roundtable was structured into two sessions: 1) an overview of the situation in DRC, including the current knowledge of epidemiology and 2) contextual considerations for response. This was followed by an hour-long panel discussion on operational considerations for response. Each session was initiated by a series of catalyst presentations followed by a question-and-answer session (Q&A). Details of the agenda, speakers and discussants can be found below.
Despite estimates that less than 10% of suspected cases in DRC are being laboratory screened, the country is currently reporting the highest number of people affected by mpox in sub-Saharan Africa. It is notable that clade 1 of mpox is linked to this outbreak, which results in more severe disease and a higher fatality rate. While early cases of mpox were reported to be in gay, bisexual, and other men who have sex with men (GBMSM), the disease is now being detected more widely in DRC. The majority of those affected are children (up to 70% by some estimates2), which is a cause for concern. The outbreak is occurring on top of an overall high burden of disease and significant challenges to the health system and humanitarian interventions.
The apparently heterogeneous picture of mpox across DRC – affecting different geographies and population groups – is shaped in part by social, economic and political factors. For instance, in South Kivu, accounts indicate that transmission via intimate and sexual contact is significant in mining areas, with an estimated one third of cases of disease reported in female sex workers. This raises questions about transactional sex and related stigma in these areas, as well as the implications of cross-border mobility linked to mining livelihoods for the spread of disease.
A history of conflict and militia activity has additional implications for humanitarian intervention and is a factor in uptake and implementation of control strategies such as vaccination. Severe limitations in government health facilities in remote areas and a plural landscape of biomedical and non-biomedical providers are additional factors to consider for patterns of care-seeking and the timely provision of biomedical care. The limited reach of formal healthcare, including surveillance, makes it difficult to estimate the extent of cases and control disease spread through conventional epidemiological strategies. There are likely further challenges in accessing less visible populations such as GBMSM, as research in Nigeria has suggested.3,4
These complex contextual realities raise significant questions for mpox response. The roundtable convened a diverse range of expertise to offer perspectives from existing research and knowledge, with an emphasis on social science evidence. This roundtable report presents a synthesised version of the roundtable discussion with additional context as needed.
Key discussion questions
- What is (un)known about the current mpox outbreak(s) in DRC and what differences are evident across regions and populations?
- What contextual social, political and livelihood factors are relevant to inform understandings of transmission and vulnerabilities in different regions and population groups?
- Are there dynamics related to stigma and/or discrimination that are relevant for RCCE, detection and care provision?
- What factors could be affecting care-seeking in different contexts and what are the implications for detection and provision of care in biomedical facilities, when appropriate and available?
- What are the challenges for rollout of ring vaccination in different regions? What learning is there from new/experimental vaccines such as for Ebola in DRC?
- What are considerations for cross-border spread and for preparedness in neighbouring countries?
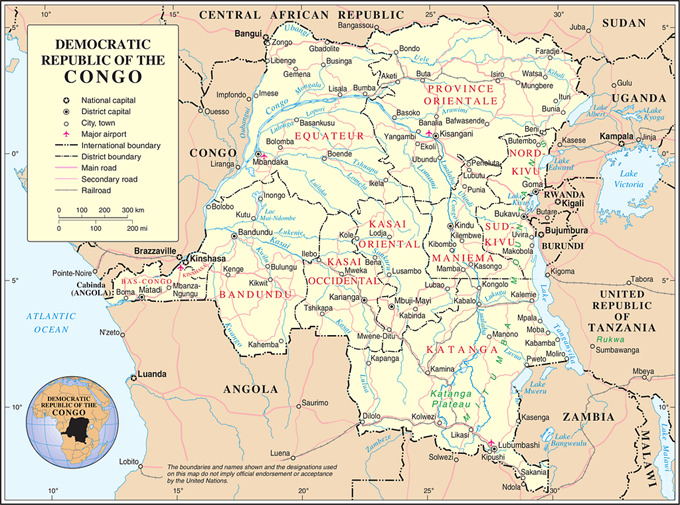
Figure 1. Map of DRC provinces
Source: United Nations: Public Domain.
Heterogeneity of the mpox outbreak/s in DRC and uncertainties
The mpox outbreak in DRC is heterogeneous and very distinct from the 2022-23 multi-country outbreak, indicating a need to understand the disease’s epidemiology in endemic regions. Mpox has been in the DRC since the virus was first identified and named in the 1970s, however the current documented outbreak(s) indicate wider spread. Research was reported from South Kivu indicating the presence of a new mpox strain, which can also be tricky to detect with some testing methods.5
Participants reported outbreak differences in the two major hotspots, one in the west and one in the east. In Équateur province, a densely forested region, cases are largely amongst children in hunting communities. There is urgent need to better understand the vulnerability of children and factors that shape the spread of mpox. Participants expressed concern was expressed that the impact on children might be underrepresented.
In South Kivu province, cases have been documented in mining towns, largely amongst female sex workers and children under the age of 15. In the mining town of Kamituga, South Kivu, cases amongst sex workers have been linked to sexual contact. Cases have also been documented in newborns, indicating vertical mother-to-child transmission of the disease. The clade I strain identified in Kamituga is virologically distinct from the clade II strain which began driving the global outbreak of mpox in 2022 and has more severe symptoms. This is based on evidence gathered by a research team operating in Kamituga.5
There are major, ongoing challenges to establishing a full picture of mpox in DRC, including issues with case identification processes, lab capacities, access to formal healthcare services and facilities, access to testing and additional challenges related to geographic and sociopolitical context which will be explored below.
Contextual factors that shape transmission and vulnerability
The mpox outbreak(s) focused in Équateur and South Kivu provinces face distinct challenges related to geographic and sociopolitical context. More social science research is needed to understand the context of mpox transmission and vulnerability amongst groups such as children in Équateur, as well as GBMSM and commercial or other transactional sex workers. In South Kivu, in eastern DRC, mpox transmission in mining towns such as Kamituga reflects intersecting challenges related to the region’s long history of conflict between armed groups, humanitarian intervention, population mobility, and resource extraction often in the form of small-scale or artisanal mining that is more informal in nature. Mpox vulnerability then reflects the intersection of livelihood seeking, transactional and professional sex work and other forms of ‘risky’ work such as mining, and healthcare seeking practices which may be shaped by emerging stigma around the disease and associated discrimination. More research is needed to understand the specific contextual factors and pathways that affect the lived experiences of people with mpox in the region.
Conflict and humanitarian intervention. One participant with expertise in humanitarian intervention in the context of conflict noted the historical context of South Kivu, where large numbers of people have been displaced since the 1990s. Armed groups such as the March 23 Movement (M23), are highly active in the Kivu region.6 Participants stressed that humanitarian organisations struggle to provide support7 as they face ongoing threats from these armed groups as well as from government forces who may be suspicious of external intervention in any form. Local and faith-based organisations are the ones who have found success in terms of providing support to local communities, as they are more trusted.8 International organisations are less trusted in this context, as is reflected in the departure earlier this year of the United Nations Organization Stabilization Mission in the Democratic Republic of the Congo (MONUSCO).9
Different forms of sex work and intersections with mining and gendered vulnerability. Another participant shed light on women’s roles in mining communities like Kamituga, where women play an integral but often marginalised role in artisanal mining. Some women are directly involved in mining activities such as polishing or crushing stones to extract minerals, but with the increasing use of machinery, fewer and fewer women are finding opportunities to do this work. Women often depend on a mining ‘site owner’ for work and may exchange sex for work opportunities. Sex work presents in different forms: professionalised or full-time sex workers or transactional sex (e.g., sex for food or goods, sex for work, or information). Some sex workers work in local bars or lodges, some are home-based sex workers and some go directly to the mining site under the supervision of a ‘godmother.’ Sex workers, like other mine workers, are highly mobile, and many may be from neighbouring regions or countries. The issue of stigma is important, including as a factor inhibiting women from seeking healthcare and instead resorting to self-care or informal providers.
Stigma and discrimination related to the outbreak
Learning from Nigeria’s outbreak for addressing mpox in ‘hidden’ populations. Findings were shared from 2022-23 social science research on mpox in southwestern Nigeria, with a focus on the heterogeneity of the situation there, with people affected representing those from different livelihoods, genders and ages. The presentation focused specifically on one aspect of that research, namely lessons learnt from participants who identified as gay or bisexual as part of the wider men who have sex with men (MSM) community. The global labelling of mpox as a disease that primarily affects MSM had implications for how MSM sought care in a country where same-sex relations are criminalised and stigmatised. In addition, those affected in Nigeria are not only from GBMSM, as has been the case in other settings in the multi-country mpox outbreak.10 This global framing of mpox as a ‘gay disease’ heightened fear and concern within the Nigerian MSM community, with misinformation spreading via social media networks about how if someone contracts mpox they ‘may die.’ It also led people with mpox to hide their diagnosis, preferring to recover at home in total isolation, without letting people in their social or sexual networks know about their experience. This pointed to the need for engagement and communication that is not alarmist, and which counteracts or avoids intensifying stigma against key groups. There is also a need to balance priorities, carefully weighing whether to focus messaging for groups which may be at ‘higher risk’ with issues of stigma and discrimination which can be worsened by that very same messaging. The vulnerability of people who are immuno-compromised, e.g. because of HIV, was noted. Finally, given this context, it is important to engage with trusted peer leaders and health workers, e.g., via specialised HIV service providers that work with ‘key populations’ to deliver sensitive information about mpox symptom identification, prevention and care.
Factors affecting detection and provision of care
The full extent of the ongoing mpox outbreak remains unknown, as many cases are likely going undetected. One participant shared several reasons for these low detection rates, which are related to socioeconomic, geographical, health system, and social factors.
Firstly, populations in affected areas have limited financial resources, making access to healthcare a significant barrier to detection and treatment of mpox. Providing free access to primary healthcare has been shown to increase the number of cases detected and treated. However, financial barriers remain a challenge for many affected populations, limiting their ability to seek care.
Limited availability of healthcare facilities is another critical issue, particularly in remote areas such as Équateur province. The affected areas are often hard to reach, with poor infrastructure and limited transportation options, making it difficult for populations to access already scarce healthcare services. This geographical barrier can lead to delayed or missed diagnoses and treatment.
Knowledge gaps about mpox among affected populations also contribute to challenges in detection and care provision. A lack of understanding about the disease symptoms and what to do when they appear can lead to delays in seeking medical attention. There are some indications that some people are turning to traditional medicine remedies or known ‘risky’ remedies instead of seeking care at healthcare facilities.
Stigma associated with mpox, particularly in areas where sexual transmission is prevalent, can hinder case detection and contact-tracing efforts. Patients may refuse to disclose their contacts due to fear of stigmatisation, making it difficult for health authorities to identify and monitor potential cases. This is especially true in regions where the disease is linked to specific groups, such as sex workers.
Insufficient testing and confirmation of cases are also contributing to uncertainties about the full extent of the mpox spread. Not enough suspected cases are being tested and confirmed, leading to an unclear picture of the outbreak’s scale. Strengthening testing capacity and case confirmation protocols is crucial for effective surveillance and response.
Finally, as noted earlier, stigma is likely playing a role in holding people back from seeking attention for their disease. This is of particular concern in areas where sexual transmission is occurring.
Considerations for mpox ring vaccination
A number of lessons can be learned from prior experiences with vaccination efforts for other disease outbreaks. One participant who studied vaccine deployments during Ebola outbreaks in Eastern DRC shared key considerations for potential future mpox vaccine interventions.
Firstly, it is important to engage communities in discussion not only about what vaccines are and how they work, but about the public health and ethical logics behind vaccine deployment strategies. During the Ebola outbreak in eastern DRC, community engagement efforts failed to dispel confusion about why certain decisions were made in relation to who did and did not receive vaccination during trials. For instance, the ring vaccination approach left many people feeling excluded from potentially life-saving treatment and, not knowing why, lead to confusion and a lack of trust. A later, second vaccine trial which took place away from the epicentre of the outbreak and with different eligibility criteria caused further confusion and reinforced this mistrust.
Lack of clarity around vaccine strategies can interact with other local realities such as limited access to healthcare and other basic services to reinforce mistrust. When households must pay for and frequently struggle to get access to routine services and care for common illnesses such as malaria, there may be suspicions about newly and freely available vaccines. This mismatch between everyday local priorities and outbreak response can further complicate efforts.
Overall, the broader political context of conflict in the DRC can also exacerbate distrust towards vaccine interventions, while vaccine efforts can also shape the political landscape. Vaccine decisions may be interpreted in political terms. Accessibility and eligibility for instance, may be perceived as reflecting political favour or disfavour of certain groups or populations, and thus influence how an intervention is received and unfolds on the ground. At the same time, vaccination efforts can also influence political context. Actors struggling for public authority may mobilise discourses around vaccination interventions to advance their own political influence.
Considerations for cross-border preparedness
Given the sociogeographical context of the current mpox outbreaks, there are concerns about cross-border spread, and the need for preparedness. Participants shared reports that spillover of mpox has already been reported in health zones in the DRC which border Rwanda and Burundi, while sex workers from these countries have been among mpox patients in Kamituga.
Risks for cross-border spread in the region include highly porous borders with weak health surveillance capacities, and highly mobile populations. Many people in the region routinely cross borders for a range of reasons including access to healthcare and other social services (e.g. for school); attending social and kinship obligations such as marriages and burials; carrying out livelihood activities such as domestic water collection, gardening/farming or visiting markets and acting on cultural beliefs and practices. For example, between Uganda and the DRC, there may be perceptions among some that healers or medicinal forest products are available and/or superior on the other side of the border. While these movements facilitate important social and economic functions for populations, they also present transmission risks.
Given this context, there is a need for improved recognition and understanding of these movements, and actions taken to address cross-border transmission. Efforts such as population mobility mapping, as has been carried out by the International Organization for Migration (IOM) in the region previously, can support this. These efforts can identify routes, movements and reasons for travel between countries. Previous efforts have not captured the movement of people traveling to engage in sex work, which may be important in the context of the current mpox outbreak. There is also a need for greater collaboration between the World Health Organization (WHO), and health ministries in Rwanda, Burundi, Uganda, South Sudan and the DRC to work together to address cross-border transmission, and to remove barriers to access to care.
Overall, there is a need for broader health system strengthening within individual countries and their sub-regions, as well as across the region. Strengthening basic services, including for routine prevention and care, as well as data collection capacities and communication from local to national and regional levels is important for enhancing preparedness and response for diseases like mpox and Ebola, while also ensuring other routine and endemic population health priorities are addressed.
Uncertainties and areas for follow-up
Despite the vast expertise shared in the roundtable discussion, the discussion also surfaced several key questions and areas for follow-up, including:
- How do we balance mpox response with the wider need for health systems strengthening?
- What are the contextual factors (social, economic, cultural, environmental etc.) shaping children’s and other groups’ vulnerability to mpox, and how might this differ in Équateur and South Kivu?
- How can we improve data sharing with centralised systems and avoid siloed approaches to research and intervention/response?
- How can we improve regional, cross-border collaboration on preparedness and response, including sharing data on mpox cases?
Participants
Speakers
- Godefroid Muzalia, Professor, Department of History and Social Science, Institut Supérieur Pédagogique de Bukavu
- Emilia Sana, Head of Planning Section, Centre des Opérations d’Urgence de Santé Publique (COUSP)
- Modeste Deffo, CP3 Country Program Manager, International Federation of Red Cross and Red Crescent Societies (IFRC) DRC
- Jean-Claude Udahemuka, Department of Veterinary Medicine, University of Rwanda
- Marie-Rose Bashwira, Associate Professor, Coordinator of the Centre for Research and Expertise in Gender and Development (CREGED-ISDR)
- Michael Kunnuji, Associate Professor, University of Lagos
- Myfanwy James, Assistant Professor in International Development and Humanitarian Emergencies, The London School of Economics and Political Science (LSE)
- Marlin Mudekereza Bisimwa, Social and Behavioral Change Communication (SBCC) Specialist, Save the Children International
- Simone Carter, Lead, Integrated Outbreak Analytics (IOA)
- Brian Ajong, Public Health Officer, WHO DRC Country Office
- David Kaawa-Mafigiri, Senior Lecturer, School of Social Sciences, Makerere University
Additional participants
- Hayley MacGregor, Professorial Research Fellow, Institute of Development Studies (IDS)
- Koen Vlassenroot, Professor of Political Science, University of Ghent
- Ancert Mushagalusa, Researcher, Catholic University of Bukavu (UCB)
- Patrice Kazadi Tshibumbu, Team Leader, Breakthrough ACTION, Save the Children International
- Lucette Womba, Global Health Security Agenda (GHSA)
- Ayodele Jegede, Professor of Medical Anthropology, Sociology and Bioethics, University of Ibadan
- Trudie Lang, Professor of Global Health Research, University of Oxford
- Pippa Ranger, Behavioural Science and Innovation Advisor, Foreign, Commonwealth & Development Office (FCDO)
- Leandre Murhula Masirika, Lwiro Natural Science Research Center
- Kit Smith, Health Security Advisor, FCDO
- Nel Druce, Senior Health Advisor, FCDO
- Kongolo Anicet, Nursing Practitioner, Bukavu/Kamituga
- Melissa Parker, Professor, London School of Hygiene and Tropical Medicine (LSHTM)
- Nadine Beckmann, Associate Professor in Social Sciences, LSHTM
- Grace Akello, Associate Professor of Medical Anthropology, Gulu University
- Megan Schmidt-Sane, Research Fellow, IDS
- Syed Abbas, Research Fellow, IDS
- Eva Niederberger, Senior Research Associate, Anthrologica
Rapporteur
- Tabitha Hrynick, Research Officer, IDS
Roundtable agenda
| Time | Topic | Speakers | |||
| 10:00 – 10:05 | Welcome | Chair: Godefroid Muzalia | |||
| 10:05 – 10:30 | Session 1. Overview of mpox in DRC
Chaired by Godefroid Muzalia Timekeeping: Syed Abbas Format: 5-minute speaker presentations and Q&A Objective: to discuss the current situation of mpox, which groups are most affected in different regions, and factors that make children vulnerable |
1. Emilia Sana – overview of mpox in DRC
2. Modeste Deffo – operational insights from Équateur on children’s vulnerability to mpox 3. Jean-Claude Udahemuka – new clade in South Kivu and insights from virological research |
|||
| 10:30 – 11:00 | Session 2. Social science insights and contextual considerations for mpox response
Chaired by David Kaawa-Mafigiri Timekeeping: Megan Schmidt-Sane Format: 5-minute speaker presentations and Q&A Objective: to share social science insights for mpox response with an emphasis on humanitarian intervention and conflict, transactional sex and livelihoods, and ‘hidden’ populations |
1. Godefroid Muzalia – humanitarian intervention and conflict in DRC
2. Marie-Rose Bashwira – context of sex work, transactional sex, and livelihoods in mining communities 3. Michael Kunnuji – ‘hidden’ populations and learning for mpox care seeking from the Nigerian mpox outbreak |
|||
| 11:00 – 11:55 | Panel discussion on operational priorities
Chaired by Michael Kunnuji Timekeeping: Hayley MacGregor Format: Questions for panellists and general discussion Objective: to discuss considerations for mpox response in DRC, with a focus on RCCE, care seeking, and cross-border contexts |
1. Myfanwy James – considerations for potential ring vaccination
2. Marlin Mudekereza Bisimwa – health communications and behaviour change 3. John Kombe, learning from the Integrated Outbreak Analytics (IOA) 4. David Kaawa-Mafigiri – cross-border transmission and preparedness in Uganda 5. Brian Ajong – priorities for response |
|||
| 11:55 – 12:00 | Closing and next steps | Chair: Godefroid Muzalia | |||
References
- WHO. (2023). Mpox (monkeypox)—Democratic Republic of the Congo. https://www.who.int/emergencies/disease-outbreak-news/item/2023-DON493
- ECDC. (2024). Outbreak of mpox caused by Monkeypox virus clade I in the Democratic Republic of the Congo. https://www.ecdc.europa.eu/en/news-events/outbreak-mpox-caused-monkeypox-virus-clade-i-democratic-republic-congo
- Schmidt-Sane, M., Abbas, S., Karam, S., & Palmer, J. (2022). RCCE Strategies for Monkeypox Response. SSHAP. https://www.socialscienceinaction.org/resources/rcce-strategies-for-monkeypox-response/
- Kunnuji, M., Schmidt-Sane, M., Adegoke, O., Abbas, S., Shoyemi, E., Lawanson, A., Jegede, A., & MacGregor, H. (forthcoming). Mpox and the MSM community in Nigeria: Exploratory insights from gay men and persons providing healthcare services to them.
- Masirika, L. M., Udahemuka, J. C., Schuele, L., Ndishimye, P., Otani, S., Mbiribindi, J. B., Marekani, J. M., Mambo, L. M., Bubala, N. M., Boter, M., Nieuwenhuijse, D. F., Lang, T., Kalalizi, E. B., Musabyimana, J. P., Aarestrup, F. M., Koopmans, M., Munnink, B. B. O., & Siangoli, F. B. (2024). Ongoing mpox outbreak in Kamituga, South Kivu province, associated with monkeypox virus of a novel Clade I sub-lineage, Democratic Republic of the Congo, 2024. Eurosurveillance, 29(11), 2400106. https://doi.org/10.2807/1560-7917.ES.2024.29.11.2400106
- Center for Preventive Action. (2024, May 15). Conflict in the Democratic Republic of Congo. Global Conflict Tracker. https://cfr.org/global-conflict-tracker/conflict/violence-democratic-republic-congo
- MSF. (2024, May 24). DRC: Civilians caught in crossfire in North and South Kivu | MSF. Medecins Sans Frontieres. https://www.msf.org/drc-civilians-caught-crossfire-north-and-south-kivu
- James, M. (2022). Humanitarian Shapeshifting: Navigation, Brokerage and Access in Eastern DR Congo. Journal of Intervention and Statebuilding, 16(3), 349–367. https://doi.org/10.1080/17502977.2021.2002591
- Nsokele, C. M., & Kika, F. K. (2024). Local knowledge and information initiatives in the conflict-affected eastern Democratic Republic of Congo. Development in Practice, 0(0), 1–15. https://doi.org/10.1080/09614524.2024.2349056
- MacGregor, H., Jegede, A., Abbas, S., Kunnuji, M., Lawanson, A., Adegoke, O., & Schmidt-Sane, M. (2023, May 12). Mpox as a public health emergency of international concern: Preparedness, priorities, politics. Institute of Development Studies. https://www.ids.ac.uk/opinions/mpox-as-a-public-health-emergency-of-international-concern-preparedness-priorities-politics/
Authors: This report was written by the Tabitha Hrynick and Megan Schmidt-Sane based on the contributions of roundtable participants.
Acknowledgements: We thank all the roundtable participants for their participation and contributions. This brief was reviewed by David Kaawa-Mafigiri (Makerere University), Syed Abbas and Hayley MacGregor (both Institute of Development Studies).
Suggested citation: Hrynick, T. and Schmidt-Sane, M. (2024). Roundtable report: Discussion on Mpox in Democratic Republic of Congo and social science considerations for operational response. Social Science in Humanitarian Action Platform (SSHAP). www.doi.org/10.19088/SSHAP.2024.014
Published by the Institute of Development Studies: May 2024.
Copyright: © Institute of Development Studies 2024. This is an Open Access paper distributed under the terms of the Creative Commons Attribution 4.0 International licence (CC BY 4.0). Except where otherwise stated, this permits unrestricted use, distribution, and reproduction in any medium, provided the original authors and source are credited and any modifications or adaptations are indicated.
Contact: If you have a direct request concerning the brief, tools, additional technical expertise or remote analysis, or should you like to be considered for the network of advisers, please contact the Social Science in Humanitarian Action Platform by emailing Annie Lowden ([email protected]) or Juliet Bedford ([email protected]).
About SSHAP: The Social Science in Humanitarian Action (SSHAP) is a partnership between the Institute of Development Studies, Anthrologica , CRCF Senegal, Gulu University, Le Groupe d’Etudes sur les Conflits et la Sécurité Humaine (GEC-SH), the London School of Hygiene and Tropical Medicine, the Sierra Leone Urban Research Centre, University of Ibadan, and the University of Juba. This work was supported by the UK Foreign, Commonwealth & Development Office (FCDO) and Wellcome 225449/Z/22/Z. The views expressed are those of the authors and do not necessarily reflect those of the funders, or the views or policies of the project partners.
Keep in touch
Email: [email protected]
Website: www.socialscienceinaction.org
Newsletter: SSHAP newsletter




![On 14 August 2018, 'Dieudonne' [not his real name], a thirteen year old boy who lost eight members of his immediate family to Ebola, stands in Ebola-affected Mangina, North Kivu, the Democratic Republic of the Congo (DRC).
“There were eight of them and they are all dead,” says Dieudonné*, a young 13-year-old boy living in Mangina, the Democratic Republic of the Congo, where 27 cases of Ebola were recently confirmed. It all started when Dieudonné’s mother fell ill and died. “When we buried Mum, the family was next to her body,” the young boy explains. “Soon after, everyone began to have headaches and diarrhoea.”
When his big sister was admitted to the Ebola treatment centre, Dieudonné stayed in the little family home alone, the same house that was the starting point of all his hardship. “Everyone who entered our home fell sick,” the boy recalls. At only 13 years of age, Dieudonné has lost all his bearings, all the people that he loved and on whom he could count. “I don’t have anyone who can take care of me anymore,” sadly explains the young boy, who does not know if his sister will survive the disease.
Dieudonné is one of 53 children orphaned by Ebola that UNICEF has identified in the east of the DRC. He currently benefits from psychosocial, material and dietary support. Dieudonné was also vaccinated against the disease a few days ago.
The young boy does not what his future will be. “I have to continue to live but I do not know how I will make it,” he explains. “This is serious.”
Following the 1 August 2018 announcement by the Government of the Democratic Republic of the Congo (DRC) of a new Ebola Virus Disease (EVD) outbreak in North Kivu, UNICEF has mobilized its teams to help contain the spread of the disease and protect children. The impact of an outbreak on children can be far reaching. It’s known from earlier outbreaks in the DRC as well as in West Africa that children can be affected in various ways. Children ca UNICEF/UN0229875/Naftalin](https://www.socialscienceinaction.org/wp-content/uploads/2018/10/UN0229875-400x200.jpg)