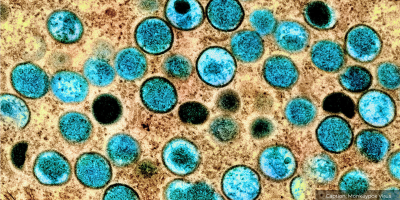
Mpox has come and gone from the international spotlight over the last few years as the first public health emergency of international concern (PHEIC) was declared in July 2022 and the second in August 2024, ending a year later. What hasn’t changed is how mpox continues to pose a risk to people in West and Central Africa, and indeed in other countries. While the ‘global emergency’ has now faded, mpox remained a continent-wide emergency until January 2026. Despite the shifting emergency declarations, lower lying levels of transmission will likely continue as mpox spreads via close contact–far too much is still unknown about the disease. The mpox outbreak(s) have demonstrated the shortcomings in our global health security system–where diseases are prioritised and de-prioritised as ‘emergencies’ and short-term thinking and short-term thinking and episodic funding cycles take precedence over longer-term health systems strengthening and health equity needs.
Scientific breakthroughs
Given this context, researchers and practitioners from the African continent came together from 3-5 December 2025 at the State-of-the-art Mpox Symposium in Kinshasa, Democratic Republic of Congo, organised by the Department of Tropical Medicine at the University of Kinshasa (UNIKIN), the Institut National de Recherche Biomédicale (INRB), the Centre for Tropical Diseases and Global Health of the Catholic University of Bukavu and the Global Health Institute (GHI) of the University of Antwerp – in collaboration with CDC Africa, WHO Africa and the Institut National de Santé Publique (INSP); and funded by the Government of Flanders. The symposium aimed to foster collaboration and share new insights on mpox. The scale and pace of scientific breakthroughs have been astonishing – from several vaccine and rapid diagnostic test candidates to potential antibody-based treatments. Social scientists are leading on efforts to understand community perspectives and engage with diverse populations as epidemic control efforts get underway.
Social science to inform effective and equitable responses
The symposium included a wide range of research projects, scientific collaborations and disciplines, showcasing latest insights on mpox endemicity, vaccines, diagnostics, epidemiology & treatment, monitoring and surveillance, prediction and control, community protection and resilience, and research capacity building. All recognised a context of sustained human-to-human transmission, reduced population immunity after routine smallpox vaccination ended, and recent genetic mutations. What emerged was a consensus that a shift is needed from mpox framed as an ‘episodic’ disease requiring isolated outbreak responses. In contrast, speakers argued for integrating mpox prevention and treatment strategies into routine care, including by exploring avenues to integrate mpox care with sexual health, HIV and primary care. Systematically including social science research enquiries will be critical to explore these pathways in a way that is centred around communities’ needs and their lived experiences of care. For instance, the discussion highlighted the need to generate evidence on pregnant women’s vulnerability to mpox, especially during the first and second trimesters, which will require a better understanding of the experiences of pregnant women and new mothers who have had/survived mpox.
We presented our recent synthesis of social and behavioural science research on mpox, which underscored gaps in the evidence base. There is a need for further investment in robust, contextually-grounded social science research to inform effective and equitable mpox response strategies in the long term. This includes stand-alone social science research as well as genuine interdisciplinary research.
Advancing an equitable research agenda
Researchers also underscored the disease’s history–mpox was seen as an ‘exotic’ disease in rural Africa by high-income and colonizing nations that posed a limited global threat since it was first identified in a lab in 1958 and amongst humans in 1970. As Nigerian scientists began to warn the global community in 2017, the disease began spreading via human-to-human contact, but it was still largely seen as a zoonotic disease limited to rural areas. The end of the first PHEIC was also seen as indication that mpox was not as much of a global priority as it should be.
Fast forward to 2025, and we still do not have viable medical countermeasures, such as scalable antiviral treatments, vaccines tested in children and pregnant women (though trials are in progress), or effective rapid diagnostic tests, tools that could prove invaluable to stopping outbreaks of the debilitating disease. Where technologies do exist, inequities in access remain. There is a need to further fund research that is testing vaccines, rapid diagnostic tests, and other biomedical priorities, but also research that understands the wider political-economic and social context of how mpox is spreading. This research agenda must be driven by and owned by Africa CDC and those on the continent.
Lessons for global health security
While mpox cases are reducing globally and indeed within West and Central Africa, there are still urgent gaps that need to be addressed. The global health community and people in power in global health institutions must meaningfully act on ‘African concerns’ as global concerns and in priority setting. Decisions to declare, lift globally (WHO) and maintain continentally (Africa CDC) the public health emergency status of mpox raise questions on what constitutes a global public health concern and whose priorities matter. Our point is that emergency declarations, and whether diseases are viewed as ‘global’ priorities, shape how and where resources are dedicated as the politics of global inequities persist. Rather than waiting until a disease has spread past controllable levels, it is important that primary health care systems are strengthened to detect and identify threats where they begin (and should end)–in communities.